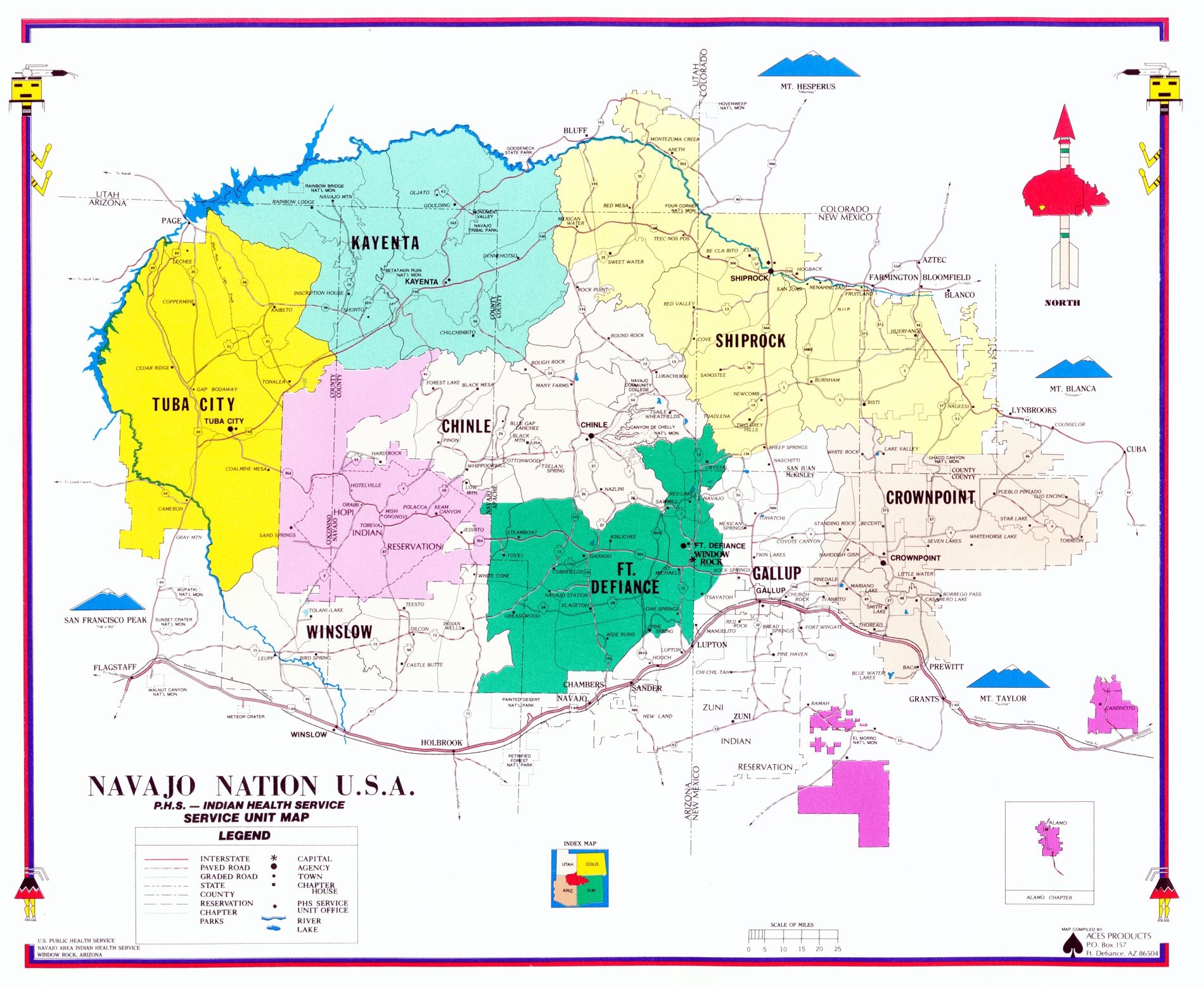
The Indian Health Service (IHS) stands as a critical pillar in the healthcare landscape for Native American and Alaska Native communities. Established to uphold the federal government’s trust responsibility, IHS delivers comprehensive health services to approximately 2.6 million eligible individuals across the United States, predominantly on or near federally recognized Indian reservations.
Understanding the IHS is more than just knowing about a government agency; it’s about recognizing a unique system born from a complex history of treaties, federal policy, and the enduring resilience of Indigenous peoples. This article delves into the intricacies of IHS, exploring its mission, the services it provides, the significant challenges it faces, and the ongoing efforts to improve health outcomes for Native Americans.
A Legacy of Trust: The Historical Context of Native American Healthcare
The foundation of the IHS is rooted in the federal government’s historical and legal obligation to provide healthcare to Native Americans. This ‘trust responsibility’ emerged from treaties and agreements where Indigenous nations ceded vast lands in exchange for various federal commitments, including provisions for health and welfare.
Initially, healthcare provisions were often sporadic and inadequate, managed first by the War Department and later by the Department of the Interior. The formal establishment of the Indian Health Service in 1955, under the Public Health Service, marked a significant shift towards a dedicated healthcare system, though its challenges were far from over.
The Indian Self-Determination and Education Assistance Act (ISDEAA) of 1975 was a landmark piece of legislation. It empowered tribes to assume control and management of federal programs, including healthcare services, previously administered by IHS. This act allowed for a move towards greater tribal sovereignty in health.
The Mission and Structure of the Indian Health Service
The primary mission of the IHS is "to raise the physical, mental, social, and spiritual health of American Indians and Alaska Natives to the highest possible level." This holistic approach recognizes the interconnectedness of well-being within Indigenous cultures.
- Directly Operated Facilities: Hospitals and clinics managed directly by IHS staff.
- Tribally Operated Facilities: Health programs managed by tribes under ISDEAA compacts or contracts.
- Urban Indian Health Programs: Non-IHS facilities funded by IHS to serve Native Americans residing in urban areas, often far from reservations.
The agency is organized into 12 administrative Areas, each overseeing a network of hospitals, health centers, and health stations. These facilities strive to provide a continuum of care tailored to the specific needs of their diverse patient populations.
Comprehensive Services for Reservation Communities
IHS and tribally operated facilities offer a broad spectrum of healthcare services. These are designed to address both acute and chronic health needs, as well as promote preventive health and wellness.
- Primary Medical Care: Routine check-ups, chronic disease management (e.g., diabetes, hypertension), and acute illness treatment.
- Dental Services: Examinations, cleanings, fillings, and extractions.
- Behavioral Health Services: Counseling, substance abuse treatment, and mental health support, often integrating traditional healing practices.
- Preventive Care: Immunizations, health screenings, and wellness programs tailored to community needs.
- Public Health Programs: Sanitation, environmental health, disease surveillance, and health education.
- Emergency Medical Services: Basic and advanced life support, often in partnership with local emergency responders.
Access to specialty care can vary significantly. For services not available at an IHS or tribally operated facility, patients may rely on Contract Health Services (CHS), which funds care purchased from private providers. However, CHS budgets are often insufficient, leading to difficult decisions about which services can be covered.
Eligibility for IHS Services: Who Qualifies?

Eligibility for IHS services is generally determined by an individual’s status as an American Indian or Alaska Native who is a member of a federally recognized tribe. While not all Native Americans are eligible, the service aims to reach those who live on or near reservations and meet specific criteria.
It’s important to note that IHS care is often provided at no cost at the point of service, but IHS facilities are increasingly billing third-party payers like Medicaid, Medicare, and private insurance. This revenue generation is crucial for supplementing congressional appropriations.
Significant Challenges: The Uphill Battle for Health Equity
Despite its vital role, the IHS system is perpetually challenged by a confluence of factors that hinder its ability to achieve health equity for Native Americans. These challenges are deeply systemic and require sustained attention and resources.
Chronic Underfunding: Perhaps the most pervasive issue is the severe underfunding of the IHS. Per capita spending on Native American healthcare is significantly lower than for other federally supported populations (e.g., Medicare, Veterans Affairs). This budget shortfall impacts everything from staffing levels to facility maintenance and the availability of specialized treatments.
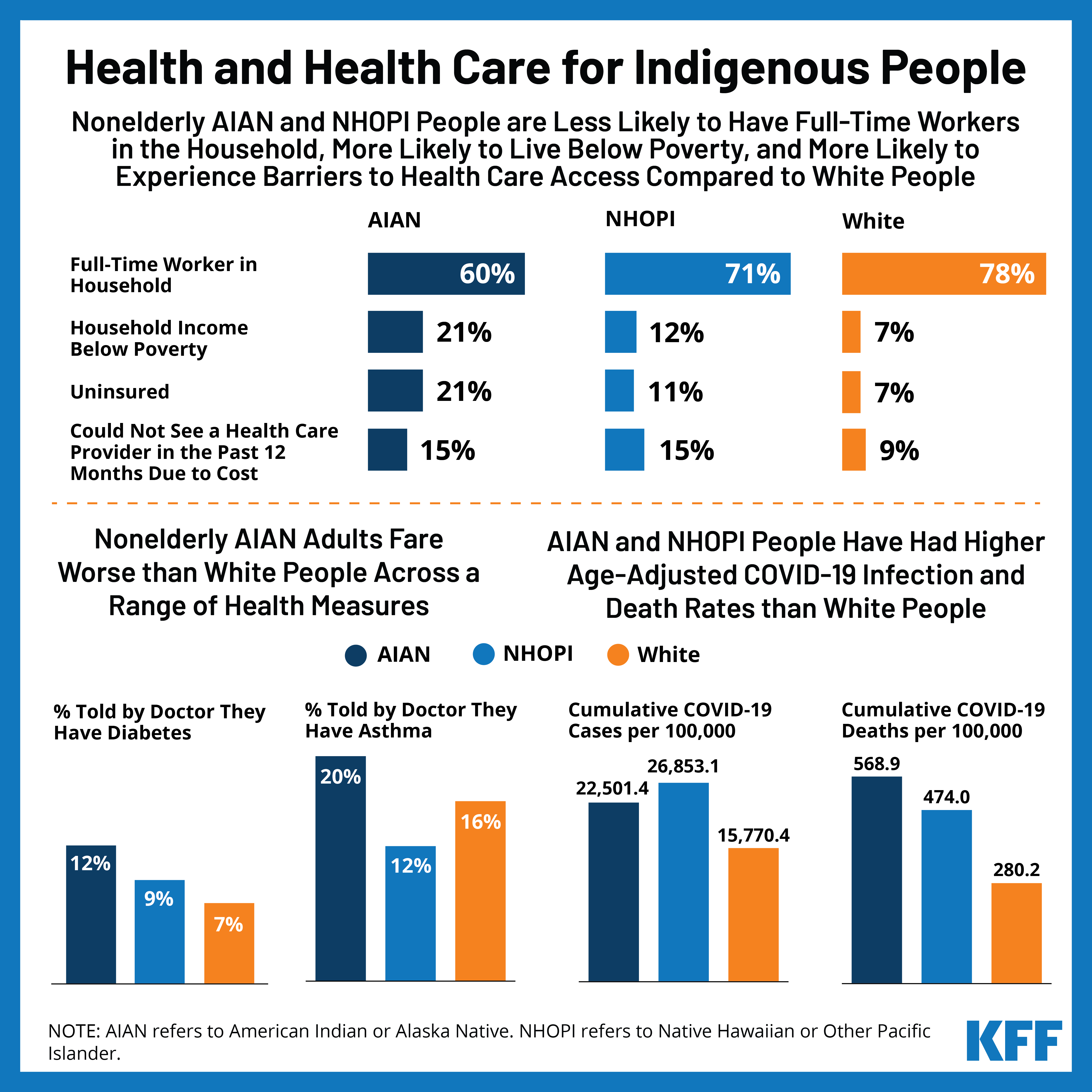
Health Disparities: Native Americans continue to experience some of the worst health disparities in the U.S. They face higher rates of diabetes, heart disease, certain cancers, unintentional injuries, suicide, and substance use disorders. These disparities are often linked to social determinants of health such as poverty, lack of education, and historical trauma.
Workforce Shortages: Recruiting and retaining qualified healthcare professionals, especially in remote reservation areas, is a constant struggle. Many IHS facilities face shortages of doctors, nurses, dentists, and mental health providers, leading to long wait times and limited service availability.
Geographic Isolation and Infrastructure: Many reservations are located in rural, isolated areas, making it difficult for patients to access specialized care or even reach primary care facilities. Aging infrastructure, including outdated clinics and hospitals, further exacerbates the problem.
Cultural Competency: While IHS strives for culturally sensitive care, there’s always a need to ensure that healthcare providers understand and respect the diverse cultural beliefs and practices of the communities they serve. Integration of traditional healing practices is an ongoing effort.
The Power of Self-Determination: Tribal Management of Healthcare
The ISDEAA has been transformative, allowing many tribes to assume direct control over their healthcare programs. This self-governance model empowers tribes to tailor services to their specific cultural values and community needs, often leading to more effective and culturally appropriate care.
Tribally managed facilities can make local hiring decisions, prioritize health initiatives, and integrate traditional healers and practices into their systems. This local control is a powerful tool for community empowerment and health improvement, though it still relies heavily on federal funding.
Innovations and the Path Forward for Indian Health
- Telehealth Expansion: Utilizing technology to connect patients in remote areas with specialists, reducing travel burdens and improving access to care.
- Community Health Representatives (CHRs): Indigenous healthcare workers who provide culturally appropriate health education, advocacy, and outreach within their communities.
- Partnerships: Collaborations with academic institutions, state health departments, and private organizations to leverage resources and expertise.
- Focus on Prevention: Increased emphasis on wellness programs, chronic disease prevention, and addressing social determinants of health.
- Advocacy for Funding: Persistent efforts by tribal leaders and advocates to secure consistent and adequate federal appropriations for IHS.
Addressing the deep-seated health disparities requires a multifaceted approach that not only strengthens the IHS but also tackles the underlying social and economic inequities faced by Native American communities.
Conclusion: A Commitment to Health and Sovereignty
The Indian Health Service on reservations represents a unique and essential component of the American healthcare system. It embodies the federal government’s enduring trust responsibility to Native American and Alaska Native peoples, striving to provide care that respects their sovereignty and cultural heritage.
While significant strides have been made, particularly through tribal self-determination, the IHS continues to grapple with profound challenges, most notably chronic underfunding and the severe health disparities that plague Indigenous communities. The journey towards health equity is ongoing.
Sustained advocacy, increased federal investment, and continued support for tribal self-governance are paramount to realizing the vision of optimal health for all Native Americans. The future of IHS must reflect a renewed commitment to justice, equity, and the inherent right to health for Indigenous nations.
The health of Native American communities is not just a tribal issue; it is a national responsibility that reflects on the commitment to human rights and the promise of a healthier future for all citizens.


