
Healthcare access on Indian Reservations in the United States presents a unique and multifaceted challenge. A complex interplay of historical factors, socioeconomic conditions, and systemic issues contributes to significant health disparities between Native American populations and the general U.S. population. This article delves into the depths of these challenges, exploring the historical context, current obstacles, and potential solutions to improve healthcare delivery on Indian Reservations.
Historical Context: A Legacy of Dispossession and Neglect
The historical relationship between the U.S. government and Native American tribes has significantly shaped the current state of healthcare access. Treaties, often broken or disregarded, established certain obligations of the federal government to provide healthcare services to Native Americans in exchange for land and resources. However, the implementation of these treaties has been inconsistent, leading to chronic underfunding and inadequate healthcare infrastructure.
The forced removal of Native Americans from their ancestral lands and placement on reservations further disrupted traditional healthcare practices and social structures. This displacement, coupled with the suppression of Native American cultures, created a climate of distrust and marginalization that continues to affect healthcare seeking behaviors today.
Current Challenges in Healthcare Access
1. Geographic Isolation and Limited Infrastructure: Many reservations are located in remote, rural areas with limited access to transportation and healthcare facilities. This geographic isolation makes it difficult for residents to reach hospitals, clinics, and specialists, especially in emergency situations. The lack of adequate infrastructure, such as paved roads and reliable communication networks, further exacerbates these challenges.
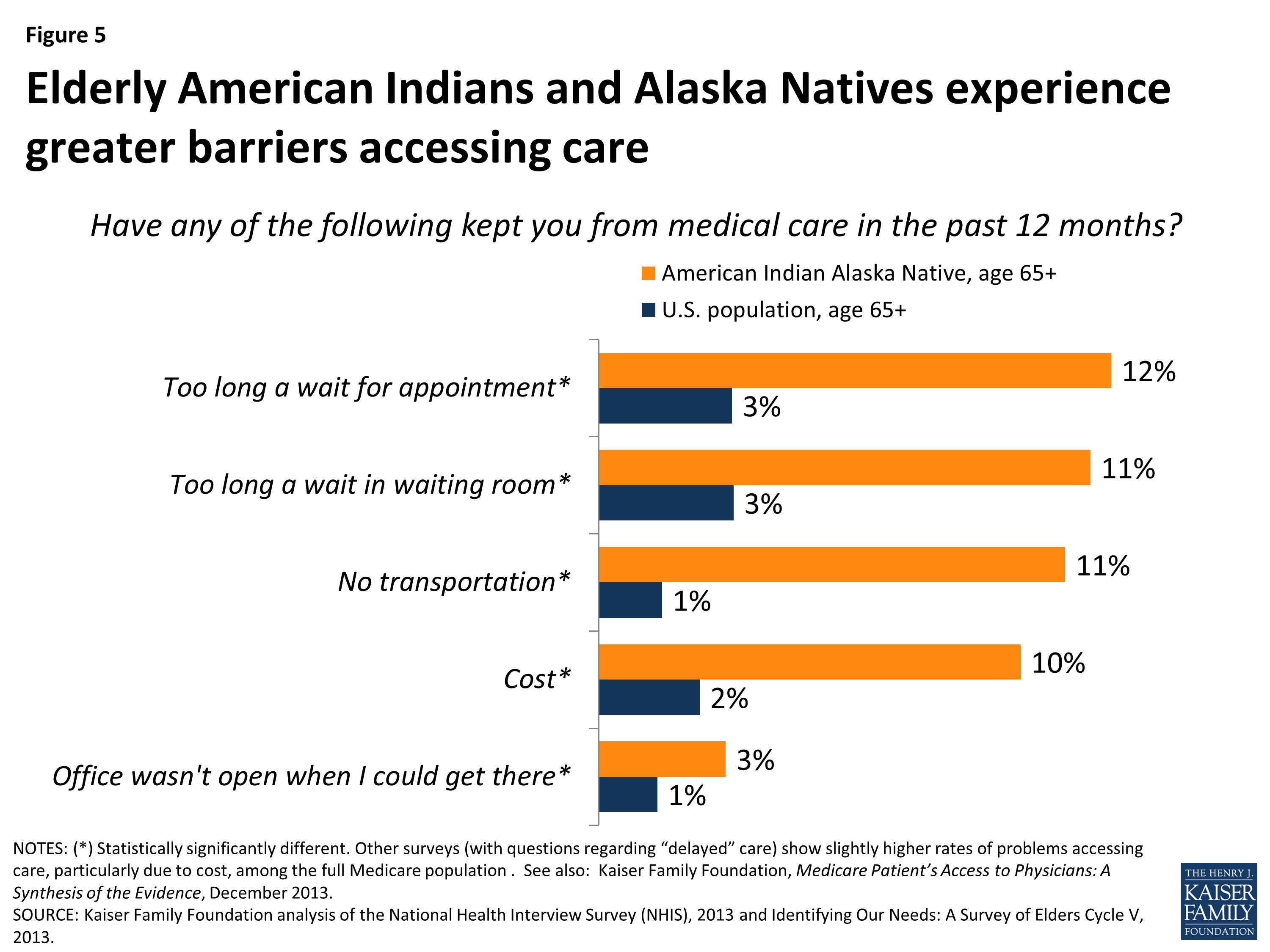
2. Underfunding of the Indian Health Service (IHS): The IHS, an agency within the Department of Health and Human Services, is responsible for providing healthcare services to approximately 2.6 million Native Americans. However, the IHS has historically been underfunded, leading to shortages of healthcare providers, long wait times for appointments, and limited availability of specialized medical services. This chronic underfunding directly impacts the quality and accessibility of healthcare on Indian Reservations.
3. Shortage of Healthcare Professionals: Recruiting and retaining qualified healthcare professionals on Indian Reservations is a persistent challenge. The remote location, limited resources, and demanding work environment often deter physicians, nurses, and other healthcare providers from practicing in these communities. This shortage of healthcare professionals further strains the already limited resources and contributes to long wait times and reduced access to care.
4. Socioeconomic Factors: Poverty, unemployment, and lack of education are prevalent on many Indian Reservations. These socioeconomic factors contribute to poor health outcomes by limiting access to healthy food, safe housing, and health insurance coverage. Additionally, stress and trauma associated with poverty and historical injustices can negatively impact mental health and contribute to chronic diseases.
5. Cultural Barriers: Cultural differences and language barriers can also impede healthcare access. Many Native Americans prefer traditional healing practices and may be hesitant to seek care from Western-trained medical professionals. Lack of culturally competent healthcare providers and interpreters can further exacerbate these barriers, leading to misunderstandings and mistrust.
6. Lack of Health Insurance: While the Affordable Care Act (ACA) has expanded health insurance coverage for many Americans, Native Americans still face challenges in accessing affordable health insurance. The complexities of eligibility requirements and enrollment processes, coupled with limited access to information and outreach services, can prevent Native Americans from obtaining the coverage they need.
Impact on Health Outcomes
The challenges in healthcare access on Indian Reservations have a significant impact on health outcomes. Native Americans experience higher rates of chronic diseases, such as diabetes, heart disease, and cancer, compared to the general U.S. population. They also have higher rates of infant mortality, suicide, and substance abuse. These disparities highlight the urgent need to address the underlying factors that contribute to poor health outcomes on Indian Reservations.
Addressing Common Questions (People Also Ask)
1. What is the Indian Health Service (IHS)? The IHS is a federal agency responsible for providing healthcare services to Native Americans and Alaska Natives. It operates hospitals, clinics, and other healthcare facilities on or near Indian Reservations.
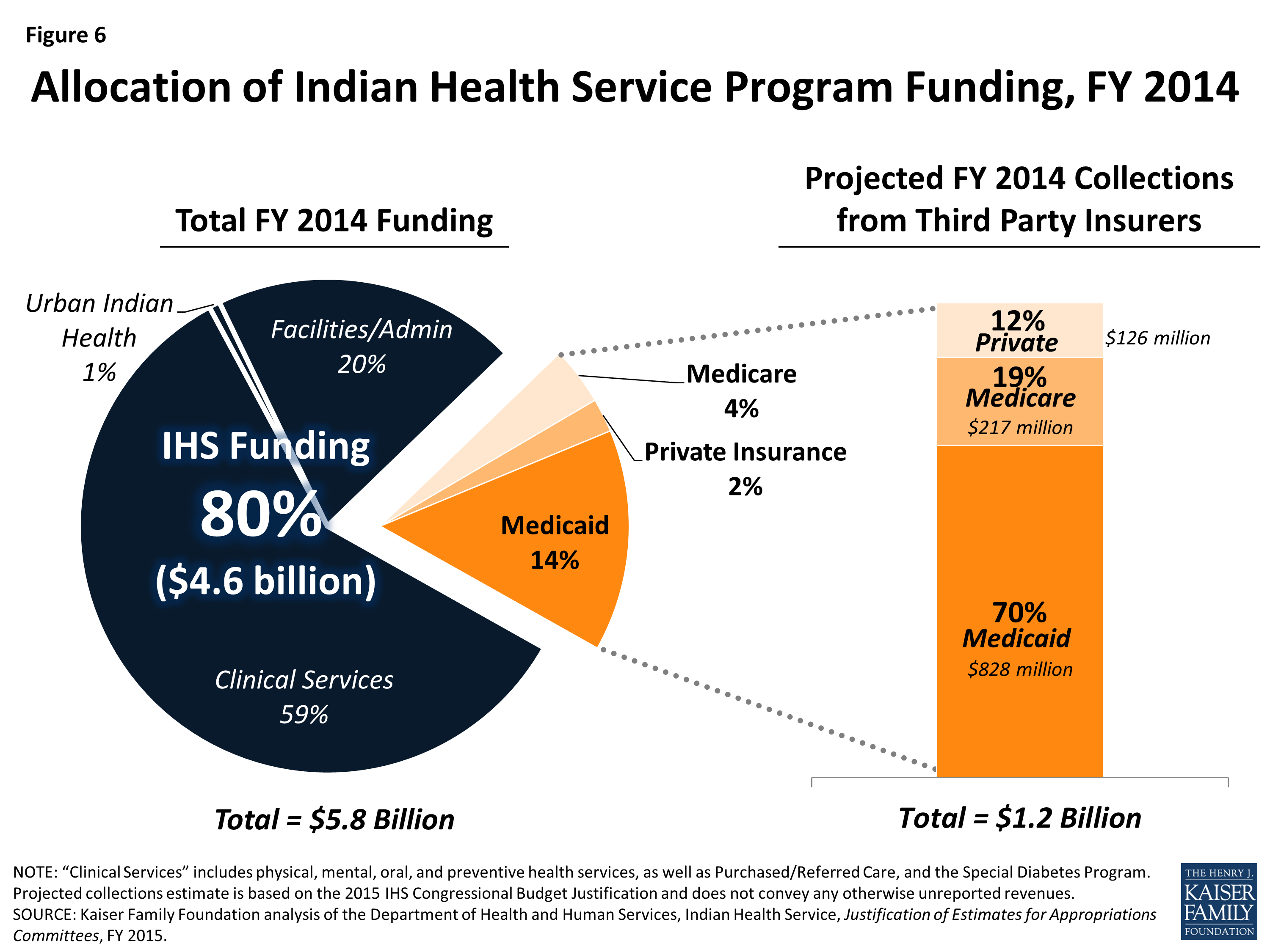
2. How is the IHS funded? The IHS is funded through congressional appropriations. However, the agency has historically been underfunded, leading to significant challenges in providing adequate healthcare services.
3. What are some of the major health challenges facing Native Americans? Native Americans experience higher rates of chronic diseases, such as diabetes, heart disease, and cancer, as well as higher rates of infant mortality, suicide, and substance abuse.
4. What are some of the barriers to healthcare access on Indian Reservations? Barriers include geographic isolation, underfunding of the IHS, shortage of healthcare professionals, socioeconomic factors, cultural barriers, and lack of health insurance.
5. What are some potential solutions to improve healthcare access on Indian Reservations? Potential solutions include increased funding for the IHS, recruitment and retention of healthcare professionals, expansion of telehealth services, culturally competent healthcare training, and addressing socioeconomic disparities.
Potential Solutions and Strategies for Improvement
1. Increased Funding for the IHS: Adequate funding is essential to address the chronic underfunding of the IHS and ensure that the agency has the resources necessary to provide comprehensive healthcare services. This includes funding for infrastructure improvements, recruitment and retention of healthcare professionals, and expansion of specialized medical services.
2. Recruitment and Retention of Healthcare Professionals: Incentives, such as loan repayment programs, scholarships, and competitive salaries, can help attract and retain qualified healthcare professionals on Indian Reservations. Creating a supportive and culturally sensitive work environment is also crucial for retaining healthcare providers.
3. Expansion of Telehealth Services: Telehealth can help overcome geographic barriers and improve access to specialty care on Indian Reservations. Telemedicine technologies can be used to provide remote consultations, monitoring, and education, reducing the need for patients to travel long distances to see specialists.
4. Culturally Competent Healthcare Training: Healthcare providers should receive training on cultural sensitivity and awareness to better understand the unique needs and preferences of Native American patients. This training should include information on traditional healing practices, language barriers, and cultural beliefs about health and illness.
5. Addressing Socioeconomic Disparities: Addressing poverty, unemployment, and lack of education is crucial for improving health outcomes on Indian Reservations. Investments in education, job training, and economic development can help create opportunities for Native Americans and improve their overall health and well-being.
6. Strengthening Tribal Sovereignty: Supporting tribal sovereignty and self-determination is essential for empowering Native American tribes to control their own healthcare systems. Tribes should have the autonomy to design and implement healthcare programs that meet the specific needs of their communities.
7. Improving Data Collection and Analysis: Accurate and comprehensive data on health outcomes and healthcare access is essential for identifying disparities and tracking progress. Improving data collection and analysis can help inform policy decisions and resource allocation.
8. Collaboration and Partnerships: Collaboration between the IHS, tribal governments, state and local health departments, and private healthcare providers is essential for improving healthcare access on Indian Reservations. These partnerships can help leverage resources, share expertise, and coordinate care.
Conclusion
Healthcare access on Indian Reservations remains a critical issue that demands urgent attention. By addressing the historical injustices, systemic barriers, and socioeconomic disparities that contribute to health disparities, we can work towards a future where all Native Americans have equitable access to quality healthcare. Increased funding for the IHS, recruitment and retention of healthcare professionals, expansion of telehealth services, culturally competent healthcare training, and strengthened tribal sovereignty are essential steps towards achieving this goal. Through collaborative efforts and a commitment to social justice, we can improve the health and well-being of Native American communities and honor the promises made to them.


